in Foot and Ankle Surgery and Reconstruction
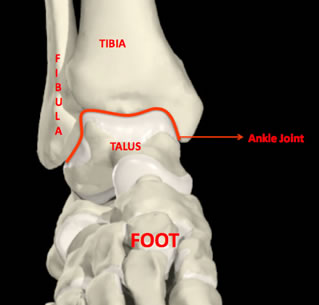
The ankle joint is the joint at the bottom of the leg between the tibia or shin bone and the talus bone in the foot. Arthritis is a condition where the smooth cartilage lining of the bones inside the joint, which allows normal smooth motion between the bones becomes worn and gradually causes friction between the bones on movement. As wear progresses the joint becomes painful.
In many patients no definite cause is found. Sometimes arthritis (wear and tear) in the joint can get gradually worse after a previous break or bad ankle sprain. People with gout or more widespread form of arthritis such as rheumatoid can develop arthritis in the ankle. Patients with bleeding disorders such as Haemophilia are more prone to arthritis developing and if you have had a previous infection in your ankle, which is unusual, you can get arthritis.
The main reason people seek medical attention is because of pain around the ankle especially on walking and exercising. There can be some swelling around the joint and in some cases quite significant stiffness. In severe cases the ankle can slowly deform, making even walking troublesome.
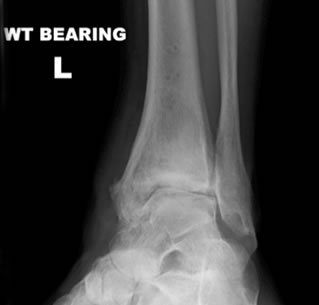
The clinical features as discussed above in addition to typical X-Ray findings seen can confirm the diagnosis. Further scans are usually unnecessary.
People often “live” with the symptoms for many years and then finally seek medical attention. If you decide not to see your doctor, the problem will tend to progress, usually slowly. Stiffness will usually increase and the pain can get worse making walking gradually more difficult and weight bearing exercise extremely difficult. The condition can be treated at any stage however early surgery can potentially preserve the joint with a joint replacement whereas later surgery may require ankle joint fusion.
The treatment is operative or non-operative.
Non-operative treatment aims to reduce the symptoms by reducing the pain on joint movement when walking. This can be through supportive boots to stabilise your ankle on walking or rocker-bottom shoes or cushioned shoes to absorb impact on walking. This is not a curative option, but may be suitable for some patients. In addition, patients may find taking pain-killers or anti-inflammatory tablets beneficial, provided there are no other medical reasons they cannot take them. Steroid injections can temporarily improve symptoms and can potentially be repeated.
Operative treatment varies depending on patient preference and expectation and the severity of the condition. In some cases the joint can be “tidied up” to restore movement. Unfortunately by improving the movement you can potentially make symptoms slightly worse, as the joint is still arthritic. This can be done via ankle arthroscopy. Alternative, more definitive options include ankle joint replacement (same concept to hip or knee replacement) or ankle joint fusion that stiffens your ankle joint permanently.
Although the joint is permanently stiffened in a fusion operation it is fixed in such a position so as to allow patients to hopefully maintain a very active lifestyle and sporting lifestyle, even jogging or running. Different shoe styles can make walking easier after a fusion. Joint replacement does aim to maintain movement however it is less predictable in its long-term outcome, especially in younger active individuals. Up to date medical literature shows that replacements are proving to be quite successful and it is a very good option to treat arthritis. As implant design progresses the success of the use of ankle replacements will continue to grow.
Many patients are simply seeking advice on managing a problem. In mild cases modifying shoes or activities can prove a successful therapy however if non-operative measures have failed to improve symptoms then surgery is indicated, but the timing of the surgery can be arranged to suit your needs. As said earlier, even if the condition worsens, surgery is always an option, but the exact surgical procedure performed may differ slightly from the original surgery possible and may be more technically challenging.