in Foot and Ankle Surgery and Reconstruction
The ankle joint is the joint at the bottom of your shin bones (tibia and fibula) and the start of your foot bones (the talus bone). Where the bones meet, the bone is covered by a smooth cartilage lining of the joint, allowing you to move the ankle normally. In people who have, for example, severe osteoarthritis, rheumatoid arthritis or possibly a previous injury or fracture of the ankle, the cartilage in your ankle joint gets damaged and gradually the space in your joint then becomes narrowed with bone on bone contact causing pain and stiffness and in some cases a deformity of the ankle develops. An ankle fusion is then performed to permanently join the damaged bones together to prevent them moving on one another and hence causing pain.
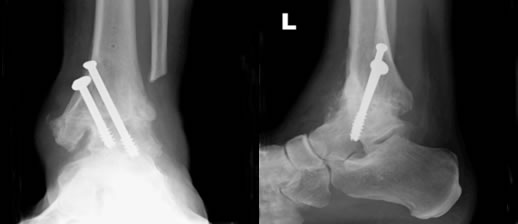
An ankle fusion is a permanent stiffening of the two main bones of your ankle joint (tibia and talus). The bones in the ankle will be held together with metal screws which act to stabilise the bones tightly together while your body naturally allows the bones to combine and fuse together. Occasionally some extra bone material is required to help with the healing. This can be taken from your own hip area or also from supplies of donor bone, stored in the hospital, however your surgeon will discuss this with you as required.
Generally 1-2 nights stay is required. The operation is done under a general anaesthesia and an added injection in the leg to numb the foot for after surgery. The operation is done minimally invasively with 2 keyhole incisions but if keyhole surgery is unsuitable then it will involve one incision usually on the outer aspect of the ankle with one extra small incision on the inside surface of the shin bone just above the ankle. The procedure involves removing the painful damaged ankle joint surfaces and then stiffening the bones together with screws or plates that stay in long term. Dissolvable skin stitches are used.
Your foot will be in a plaster cast to the knee, numb and pain free. You will see a physiotherapist who will advise on walking non-weight bearing. You will be discharged only when comfortable and given an out-patient appointment and pain-killers as required.
Your physiotherapist will guide you through the stages of rehabilitation including gait re-education, swelling reduction and reducing muscle tightness. It is important to adhere to advice given.
Keep the plaster cast totally dry. You may shower with a waterproof cover over the plaster. Once the plaster is removed you may shower if the wound is healed by carefully removing the boot and gently dab the wound dry.
Once out of cast, do not pull at scabs but let them fall away naturally. If your wound becomes red, swollen or sore you need to see your Consultant to ensure there is no infection present. Your physiotherapist may advise on wound massage when its healed.
DVLA states it is the responsibility of the driver to ensure they are always in control of the vehicle. A good guide is if you can stamp down hard with the foot to stop the car in an emergency stop. This will take at least 12 weeks. Click here to read DVLA guidance.
This is very individual and job-dependent. Below is a guide:
Excellent pain relief on mobilising is noticed early on and will improve rapidly as the bones fuse after 3 months. Good function on walking and activity is expected by 6 months and after 12 months return to full level of activity is expected. Some swelling may remain in your foot and ankle for 12 months. Your walking should be markedly improved, however the way you walk may change very slightly because your ankle will now be totally stiff. Over 90% of people generally are very, very happy and can still perform many physical/sporting activities. It is a great operation to perform.
Any operation carries a risk. Below is a guide to some risks potentially encountered. It is the surgeons duty to fully inform you of possible risks. Mr Roche will ensure this is always done so patients can make safe and informed choices about their operation.
If this happens, it is usually simply treated with antibiotics. Significant consequences are potentially serious but rare and can be dealt with by further surgery. The risk is around 1%.
Nerves that supply sensation to the skin are near the incision site. Damage is rare but if your toe stays numb after surgery, the nerve may be bruised. If so it usually recovers. The risk is <5%
This means the bones fail to biologically fuse. Occasionally it can be “painless” and intervention may not be needed unless deformity develops. If painful, then treatment options will be discussed. The risk is 5-10%
Sometimes the metal can be prominent and once the bones have fused, usually after 6-12 months the metal can easily be removed with a small day-case operation.
Symptomatic clot formation in the leg is fairly unusual after ankle surgery (<5%). You may be given blood-thinning medication after the surgery if the surgeon deems you to be a higher risk.
Certain things may delay or even prevent the bones from fusing together. You must try to avoid them. This includes:
This document is only meant to be a guideline to help you understand your treatment and what to expect. Every person is different and your rehabilitation may be quicker and slower. This will be advised and guided by your doctor and physiotherapist.