in Foot and Ankle Surgery and Reconstruction
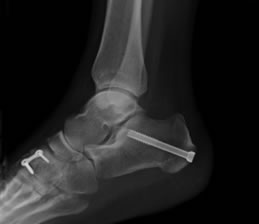
Generally 1 night hospital stay is required. The operation is done under a general anaesthesia and an added injection in the leg to numb the foot for after surgery. The operation in general will involve 3 incisions on the foot. The procedure involves removing the painful damaged tendon on the instep and substituting it with a tendon close-by called the FDL (flexor digitorum longus) tendon. To assist the newly transferred tendon we routinely perform one other operation called a calcaneal osteotomy. This is a purposely-made cut in the heel bone (osteotomy), to allow us to reposition the heel bone slightly and fix with a metal screw. By repositioning the heel bone it helps improve the support to the arch of your foot. To place the screw a small incision is made on the back of the heel and another incision is made on the outside of the heel bone to reposition the heel bone. Sometimes an added operation is done on the middle of the foot to put a small plate on the top of the foot to increase the arch of the foot, but if needed your surgeon will explain this to you beforehand. Dissolvable skin stitches are used.
Your foot will be in a plaster cast to the knee, numb and pain free. You will see a physiotherapist who will advise on walking non-weight bearing. You will be discharged only when comfortable and given an out-patient appointment and pain-killers as required.
Your physiotherapist will guide you through the stages of rehabilitation including gait re-education, swelling reduction and reducing muscle tightness. It is important to adhere to advice given.
Keep the plaster cast totally dry. You may shower with a waterproof cover over the plaster. Once the plaster is removed you may shower if the wound is healed but gently dab the wound dry.
Once out of cast, do not pull at scabs but let them fall away naturally. If your wound becomes red, swollen or sore you need to see your Consultant to ensure there is no infection present. Your physiotherapist may advise on wound massage when it has healed.
DVLA states it is the responsibility of the driver to ensure they are always in control of the vehicle. A good guide is if you can stamp down hard with the foot to stop the car in an emergency stop. This will take at least 8 weeks. Click here to read DVLA guidance.
This is very individual and job-dependent. Below is a guide:
Good level of activity and sports by 6 months to continue to improve consistently up to 12 months. Insoles can be used long-term to better confidence in sporting and daily activities if necessary. Some swelling may remain in your foot and ankle for 12 months following surgery.
Any operation carries a risk. Below is a guide to some risks potentially encountered. It is the surgeons duty to fully inform you of possible risks. Mr Roche will ensure this is always done so patients can make safe and informed choices about their operation.
If this happens, it is usually simply treated with antibiotics. Significant consequences from infection are very rare but can be dealt with. Risk is around 1%.
Nerves that supply sensation to the skin are near the incision site. Damage is rare but if your toe stays numb after surgery, the nerve may be bruised. If so it usually recovers. Risk is around 5%.
In severe cases, rarely symptoms persist. If this happens your surgeon will discuss the options that could include long-term orthotics/insoles or further surgery.
Sometimes the metal can be prominent in the heel, and, usually after 6 months the metal can easily be removed with a small day-case operation.
Symptomatic clot formation in the leg is unusual after ankle surgery (<3%). Whether treatment to prevent clot is needed can be discussed with your surgeon. There is no consensus amongst UK Orthopaedic surgeons as to whether preventative medicine is needed.
This document is only meant to be a guideline to help you understand your treatment and what to expect. Every person is different and your rehabilitation may be quicker and slower. This will be advised and guided by your doctor and physiotherapist.