in Foot and Ankle Surgery and Reconstruction
Ankle arthroscopy allows the surgeon to inspect you ankle inside. Your surgeon has usually diagnosed the problem before the surgery with scans and examination and is not just looking inside to see what may be wrong.
Things you can treat with arthroscopy:
Painful overgrowth of bone or ligament/scar tissue often on the front of the ankle that is painful on joint movement
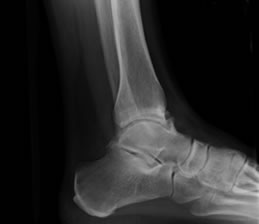
Painful rubbing in the ankle of the ligaments/scar tissue between the bottom of the fibula and tibia bones. The inflamed tissue can be safely removed.
A small defect in the soft cartilage lining of the joint from an injury that can cause pain, catching, giving way or swelling. The small defect can be treated to try to return the joint lining to normal and restore function.
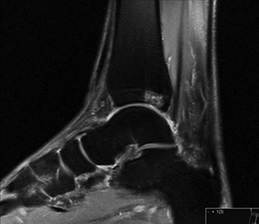
General wear and tear pain can be potentially improved with arthroscopy but the success is dependent on the degree of initial damage.
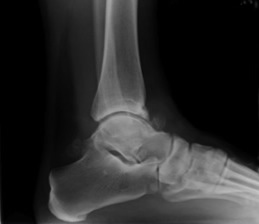
Bits of bone or cartilage can sometimes float around the ankle causing catching, pain and swelling. They are usually caused by an old injury.
It is a daycase operation. The operation is done under a general anaesthesia and an added injection in the ankle to numb it for after surgery. The operation itself involves 2 keyhole incisions on the front of the ankle or sometimes on the back of the ankle which will be explained to you by the surgeon. Depending on what the diagnosis is from the list above, the surgeon uses small instruments through the incisions, whilst looking at a monitor attached to tiny camera placed into the ankle through one of the incisions. They then carefully perform the procedure, removing scar tissue or tidying up the cartilage as required. Skin stitches are used, that will need removing after 2 weeks.
Your foot will be bandaged, numb and pain free. You will see a physiotherapist who will advise on movements and walking. Your instructions on weight bearing will be given to you by the physio after surgery because it really depends on the exact procedure the surgeon preformed in your ankle. You will be discharged only when comfortable and given a follow-up appointment and pain-killers as required.
In contrast to most foot and ankle operations, the walking instructions will depend on exactly what is done inside your ankle during the operation. Below is a guide:
In the first 2 weeks keep the bandaging/foot totally dry. You may shower with a waterproof cover over the leg. After 2 weeks you can only shower if the wounds are healed but gently dab the wounds dry.
Remove the bandage after 5 days and replace it with a elastic compression bandage (tubigrip) but keep the small sticky dressings on the wound. A district nurse/local surgery can facilitate this if needed. Once out of bandaging, do not pull at scabs but let them fall away naturally. If your wound becomes red, swollen or sore you need to see your Consultant to ensure there is no infection present. Your physiotherapist may advise on wound massage.
Your physiotherapist will guide you through the stages of rehabilitation including gait re-education, ankle mobilisation exercises, swelling reduction and reducing muscle tightness. It is important to adhere to advice given.
DVLA states it is the responsibility of the driver to ensure they are always in control of the vehicle. A good guide is if you can stamp down hard with the foot to stop the car in an emergency stop. This will take at least 2 weeks but if you had an OCD debridement it will be at least 6 weeks. Click here to read DVLA guidance.
This is very individual depending on the surgery performed and job-dependent. Below is a guide:
The outcome will depend on the severity of the condition and the exact operation carried out. In general you should be back to full activity and sports within 3-6 months. Ankle swelling can persist for 6 months or more.
Any operation carries a risk. Below is a guide to some risks potentially encountered. It is the surgeons duty to fully inform you of possible risks. Mr Roche will ensure this is always done so patients can make safe and informed choices about their operation.
If this happens (<1%), it is usually simply treated with antibiotics. Significant consequences from infection (<0.5%) are very rare but can be dealt with.
Small nerves that supply sensation to the skin are near the incision site. Damage is rare (<2%) but if your toe stays numb after surgery, the nerve may be bruised. If so it usually recovers.
Symptomatic clot formation in the leg is unusual after keyhole surgery (<1%). You can reduce the likelihood of clot forming if you maintain limb movement and perform exercises given to you by the therapists.
This document is only meant to be a guideline to help you understand your treatment and what to expect. Every person is different and your rehabilitation may be quicker and slower. This will be advised and guided by your doctor and physiotherapist.