Plantar Fasciitis or Heel Pain
What is Heel pain?
A traditional term for a common painful problem of the heel is “policemans heel” from prolonged “walking the beat”. This pain and inflammation is called “Plantar Faciitis”.
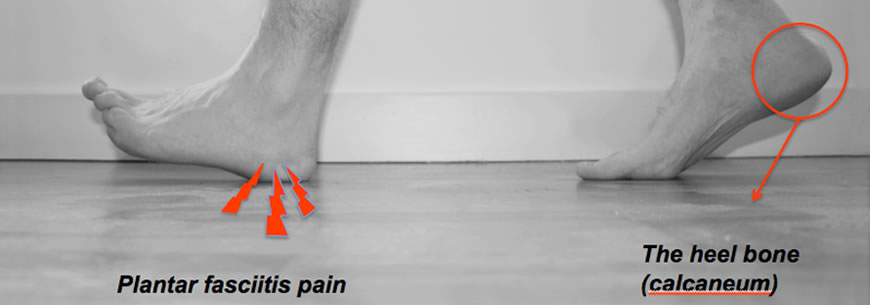
What causes Heel pain?
Probably the commonest cause of troublesome heel pain is plantar fasciitis. Other causes include:
- Calcaneal bone stress fracture
- Irritation of small nerves around the heel
- Thinning of the protective pad/tissue on the heel
What is plantar fasciitis?
Plantar means sole or bottom of foot, fasciitis refers to inflammation of the fascia. Fascia is a thick lining of the sole of the foot that runs from the heel to the toes.
What can contribute to plantar fasciitis?
- Mechanical imbalances in the foot such as high arched or flat feet
- Hard soled or non-supportive shoes.
- Regular long distance walking, performing sports on hard surfaces
- Increased body weight
- Reduced calf and hamstring muscle length, and restricted ankle joint movement
What are the symptoms?
- Heel pain. If this thick band of fascia is repeatedly placed under pressure or overloaded, degenerative changes may occur within the tissue.
- Pain may also be felt in the arch of the foot region.
- Pain is often worse when first standing after resting, typically getting out of bed.
How is the condition diagnosed?
The clinical features as discussed above along with an accurate examination by the surgeon can usually make the diagnosis. An X-Ray is not routinely required.
What if I have a bone spur?
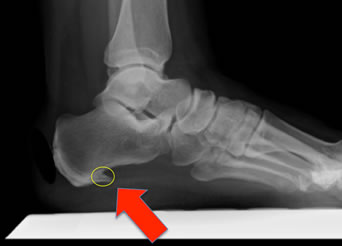 If an X-Ray was done for some reason, and a bone spur is seen on it, it is important to understand that this does not usually cause the pain, it is normally a coincidental finding. The bone spur refers to a small protruding spike of bone directly under the sole of the heel, not on the back of the heel.
If an X-Ray was done for some reason, and a bone spur is seen on it, it is important to understand that this does not usually cause the pain, it is normally a coincidental finding. The bone spur refers to a small protruding spike of bone directly under the sole of the heel, not on the back of the heel.
IF THIS IS SEEN ON AN X-RAY IT IS OF NO CONSEQUENCE AND DOES NOT NEED TO BE REMOVED.
Can the problem get worse?
People often “live” with the symptoms for many years and then finally seek medical attention. If you decide not to see your doctor, the problem will tend to persist, with no other consequence, but some discomfort and pain may continue. On the other hand, the condition can be self limiting and resolve itself but may take over 18 months.
How do you treat Plantar fascitis?
The vast majority of cases are treated non-operatively. Invariably a combination of therapies are used to treat the symptoms:
- Physiotherapy
Specific stretches and exercises can have a dramatic benefit to the symptoms, but need to be performed regularly as instructed
- Night splints
Easy to wear splints can hold your foot pulled upwards in bed while you sleep, so that when you awaken your symptoms on putting your foot down onto the floor can be improved
- Insoles/heel pads
Shock absorbing heel pads or special insoles to reduce the sharp pain in your foot on walking can alleviate your symptoms
- Shock wave therapy
In cases where the other therapies have failed to improve the symptoms then shock wave can be used. Some studies have shown reasonable success with this treatment, and its use is showing good promise.
- Steroid injections
Injection success is unpredictable, it is easy to administer but carries small risk of infection, increased pain and damage to heel-pad tissues. It can be tried, again after alternative therapies have been unsuccessful.
- Surgery
An operation can be performed if symptoms are significant and persistent for over 12 months despite ALL other modes of treatment. The operation is infrequently required and like steroid injections, is a little unpredictable in its success/failure, with about 60% of operations providing favourable results.
Deciding whether surgery is necessary
Many patients are simply seeking advice on managing a problem. In some cases modifying shoes/insoles or non-invasive therapy can prove a success however if not then surgery can be discussed, but the timing of the surgery can be arranged to suit your needs.

 If an X-Ray was done for some reason, and a bone spur is seen on it, it is important to understand that this does not usually cause the pain, it is normally a coincidental finding. The bone spur refers to a small protruding spike of bone directly under the sole of the heel, not on the back of the heel.
If an X-Ray was done for some reason, and a bone spur is seen on it, it is important to understand that this does not usually cause the pain, it is normally a coincidental finding. The bone spur refers to a small protruding spike of bone directly under the sole of the heel, not on the back of the heel.